You’ve heard the modern aphorism that it’s better to act now and ask forgiveness later than it is to ask permission and risk being denied. Well, that may work for some people in some situations; but it won’t work in the setting and circumstance described hereinbelow. In fact, it will cause you to crash and burn.
Mother, May I?
It is interesting how childhood diversions prepare us for grownup life, such as the game where kids have to politely ask permission of a designated “mother” before proceeding forward. While adults may no longer need to get their mother’s permission before acting, the nanny state still imposes a certain stringency upon its subjects. That is, in some circumstances, the government still requires you to be on your Ps and Qs, to say please and to get prior approval.
The Centers for Medicare & Medicaid Services (CMS) has something known as the Hospital Outpatient Department (OPD) Prior Authorization program, first implemented in July 2020. According to the program’s website:
CMS believes prior authorization for certain hospital OPD services will ensure that Medicare beneficiaries continue to receive medically necessary care while protecting the Medicare Trust Fund from improper payments and keeping the medical necessity documentation requirements unchanged for providers.
So, the whole point of the program is to preemptively deny payment for certain procedures CMS has previously determined to be dubious or potentially tenuous in terms of the medical necessity threshold. They want you to get prior permission before proceeding with the service. Otherwise, you invite a big fat denial upon the submission of your claim.
CMS maintains a list of medical services and procedures performed in the hospital OPD that are subject to the prior authorization requirement. These include the following:
- Blepharoplasty
- Botulinum toxin injection
- Rhinoplasty
- Panniculectomy
- Vein ablation
- Cervical fusion with disc removal
- Implanted spinal neurostimulators
The Prior Authorization program does not create new documentation requirements, per se. Rather, the documentation required to be included with a prior authorization request is information that hospital OPDs are regularly required to maintain for Medicare payments. For specific documentation details, go the applicable program website: Prior Authorization for Certain Hospital Outpatient Department (OPD) Services | CMS.
Expanding the List
The Hospital OPD Prior Authorization program has added a new service category to its list of medical services and procedures subject to the prior approval mandate. According to the program’s website, “For dates of service beginning on or after July 1, 2023, the following additional hospital OPD service category will be required as a condition of payment: Facet Joint Interventions.” In the event there is some confusion as to what specific services “facet joint interventions” entail, here is a list of applicable codes and corresponding descriptors as supplied by CMS’ guidance on this matter (Transmittal 11753):
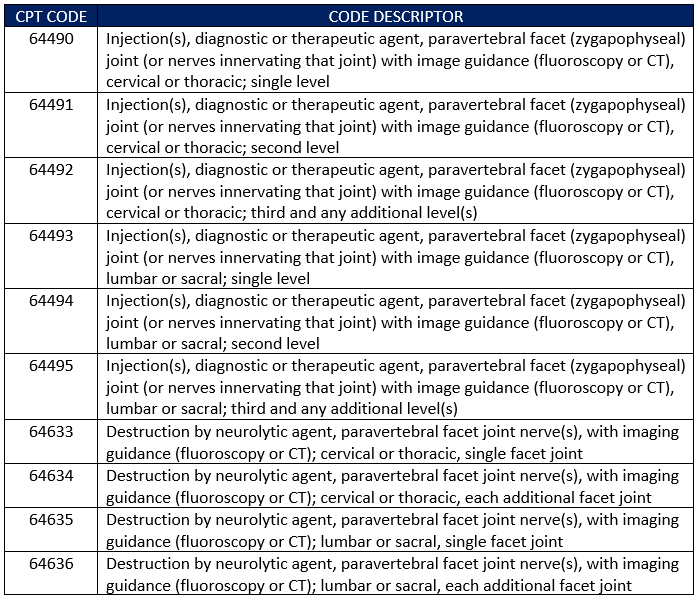
A Look at the Process
As it concerns the obtaining of prior authorization for these facet-related services, as well as the other services previously listed, the request must be submitted by the hospital OPD, the OPD physician, or other third party on behalf of the OPD, referred to as a “requester.” Under the Prior Authorization process, the requester must submit the request with the required documentation before the service is rendered. If a provider is currently exempt from OPD prior authorization process, that provider should not submit prior authorization requests, including those dealing with facet joint interventions.
After receipt of all required documentation from the requester, your regional Medicare administrative contractor (MAC) will review the prior authorization request and issue a provisional affirmation or non-affirmation within ten (10) business days of receipt. (A provider may request an expedited review if the beneficiary’s life, health, or ability to regain maximum function is in jeopardy.)
If the prior authorization request is not approved by your MAC, the requester may revise and resubmit the request an unlimited number of times. The MAC will review and communicate a decision within ten (10) business days on each resubmitted prior authorization request, providing detailed reasons for the non-affirmation decisions, as well as offering education to help the provider resolve any underlying issues.
So, like any good parent who doesn’t just deny you permission but tells you why, so CMS issues a rationale for its rejections of providers’ prior authorization requests. Nevertheless, all this acts as a stark reminder that not all supplications we submit to the government are going to be granted—no matter how politely we ask. Sometimes, Mother says “no.”
With best wishes,
Chris Martin
Senior Vice President—BPO
